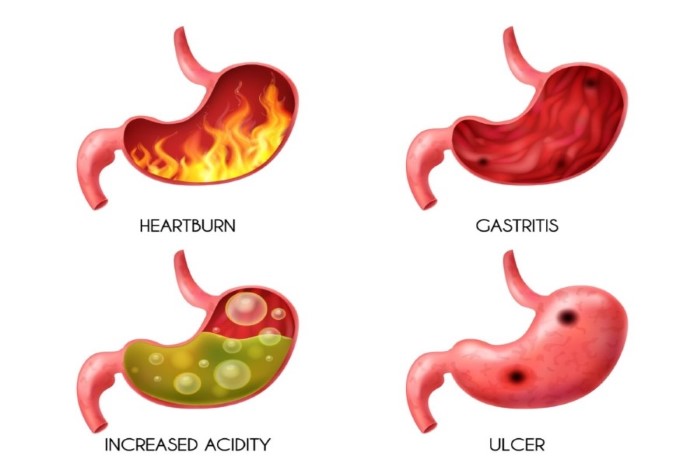
Before using medication to treat gastroesophageal reflux, it may be beneficial to make a few lifestyle changes.
If you have a painful throat and a somewhat hoarse voice, you may be getting ready for the flu or a cold. However, if you’ve experienced these symptoms for some time, it’s possible that your lower esophageal sphincter, a valve, is to blame rather than a virus. That particular muscle regulates the opening between the oesophagus and the stomach, and if it doesn’t shut all the way, food and stomach acid can flow back into the oesophagus. Acid reflux is the backward flow of acid, and gastroesophageal reflux is the medical term for this ailment.
You may get a bitter aftertaste in your mouth, sore throats, and hoarseness as a result of acid reflux. When acid reflux results in ongoing symptoms, it is referred to as gastroesophageal reflux disorder (GERD). Heartburn, which manifests as chest and upper abdominal pain, is the most typical symptom of GERD.
Acid reflux is caused by three factors: inadequate stomach acid production, inadequate food or acid clearance from the oesophagus, and delayed stomach emptying.
If you experience frequent heartburn or any other acid reflux symptoms, you might want to try the following advice given by our expert doctors at Marinas Clinic.
Eat little and frequently:
There may be greater reflux into the oesophagus when the stomach is really full. You might want to give “grazing,” or eating smaller meals more frequently rather than three meals a day, a try if it works with your schedule.
Avoid certain foods:
All except the blandest foods were traditionally advised to be avoided by those with acid reflux. But that’s not the case now. According to Dr. Preethi, our chief Surgeon at Marinas Clinic, “We’ve changed from the times when you couldn’t eat anything.” However, some foods continue to be more likely to cause reflux than others, such as mint, fatty meals, spicy foods, tomatoes, onions, and garlic, as well as coffee, tea, chocolate, and alcohol. If you routinely consume any of these items, you might try cutting them out to see if doing so reduces your reflux. If it does, you might then try bringing them back one at a time.
A big NO for carbonated beverages:
They cause burping, which opens the oesophagus to acid. Use still water in place of sparkling water.
Keep awake after eating:
While standing or even seated, gravity alone helps keep stomach acid where it belongs. Finish eating three hours before going to bed. This forbids snoozes in the afternoon, late supper, and midnight snacks.
Don’t go too quickly:
Avoid any vigorous activities for a few hours after eating. Walking after supper is acceptable, but strenuous exercise, especially if it involves bending over, can result in acid entering the oesophagus.
Lie down inclined:
Your head should be 6 to 8 inches higher than your feet in ideal circumstances.’Extra-tall’ bed risers can be used to achieve this by mounting them on the bed’s head support legs.. If your bed partner doesn’t like the change, think about using a foam wedge to support your upper body. Avoid attempting to construct a wedge by stacking cushions.Don’t attempt to stack pillows to form a wedge. They won’t provide you with the ongoing assistance you need.
If instructed, reduce your weight:
Gaining weight reduces the pressure that keeps the lower esophageal sphincter closed by dispersing the muscles that support it.
Quit smoking if you do:
The lower esophageal sphincter may relax as a result of nicotine.
Examine your prescriptions:
The sphincter can be relaxed by some medications, such as postmenopausal oestrogen, tricyclic antidepressants, and anti-inflammatory pain relievers, while the oesophagus can become irritated by others, particularly bisphosphonates like alendronate (Fosamax), ibandronate (Boniva), or risedronate (Actonel), which are used to increase bone density.
As per our experts’ suggestion consult your doctor to rule out other causes if these measures don’t work or if you experience significant discomfort or trouble swallowing. Even if you make lifestyle modifications, reflux may still need to be treated with medication.
© 2024 Marinas Clinic All rights reserved.Powered by Zero Gravity Technologies.