Effective Approaches to Managing Chronic Acid Reflux

Effective Approaches to Managing Chronic Acid Reflux Introduction Battling chronic acid reflux can be challenging, disrupting comfort and daily routines. At Marina’s Clinic in Chennai, Dr. Preethi, a highly skilled gastro surgeon specialising in laparoscopy and minimal access techniques, offers comprehensive and individualised solutions for managing digestive conditions. This post explores Dr. Preethi’s innovative strategies, highlighting laparoscopic fundoplication as a one-day stay procedure for managing chronic acid reflux, and presenting a roadmap to enhanced digestive health and well-being. Understanding Chronic Acid Reflux with Dr. Preethi Chronic acid reflux, or gastroesophageal reflux disease (GERD), is a condition where stomach acid frequently flows back into the oesophagus, causing irritation and discomfort. At Marina’s Clinic, Dr. Preethi, our esteemed gastro surgeon, employs minimal access techniques and laparoscopy to provide expert care and tailored treatments for managing digestive conditions, including chronic acid reflux. 1. Dr. Preethi’s Lifestyle Modification Recommendations for Minimal Access Dr. Preethi emphasises the role of lifestyle modifications as a foundational approach for managing chronic acid reflux. By adopting healthy habits such as maintaining optimal weight, avoiding trigger foods, and consuming smaller, balanced meals, patients can experience significant relief. These strategies, coupled with minimal access interventions, form the backbone of treatment at Marina’s Clinic. 2. Medication Management and Laparoscopy by Our Gastro Surgeon Dr. Preethi, renowned for her expertise in gastro surgery and laparoscopy, underscores the importance of effective medication management in controlling acid reflux symptoms. A combination of over-the-counter antacids, H2 blockers, and proton pump inhibitors can neutralise or reduce stomach acid production, ensuring optimal digestive health. 3. Nutritional Strategies and Minimal Access Techniques Advocated by Dr. Preethi Balancing your diet is essential in managing chronic acid reflux. Dr. Preethi advocates for a diet rich in high-fibre foods, lean proteins, and alkaline components to harmonise stomach acidity. Avoiding irritants like spicy foods, caffeine, and alcohol, alongside minimal access interventions, can contribute to maintaining digestive health. 4. Laparoscopic Fundoplication by Surgeon Dr. Preethi When conventional interventions prove insufficient, Dr. Preethi recommends laparoscopic fundoplication, a minimal access surgical procedure. This innovative technique strengthens the lower esophageal sphincter and is performed as a one-day stay at Marina’s Clinic, highlighting our commitment to patient convenience and advanced care. 5. Stress Management for Enhanced Digestive Health through Minimal Access Incorporating relaxation techniques such as deep breathing, meditation, and regular exercise is paramount in managing stress, which can exacerbate acid reflux symptoms. Dr. Preethi champions these practices along with minimal access techniques to form a holistic approach to digestive health. 6. Regular Monitoring and Follow-ups: A Proactive Approach with Laparoscopy Under Dr. Preethi’s vigilant care and expertise in laparoscopy, emphasising regular check-ups and follow-ups at Marina’s Clinic ensures the effectiveness of your treatment plan and allows for timely adjustments, providing an opportunity for addressing any concerns promptly. Conclusion: Dr. Preethi, a renowned gastro surgeon at Marina’s Clinic, combines her expertise in laparoscopy and minimal access techniques to offer innovative and effective solutions for managing chronic acid reflux. Our commitment to advanced care, including one-day stay laparoscopic fundoplication, fosters your journey towards optimal digestive health. Contact Marina’s Clinic Today! Ready to take a step towards better digestive health with Dr. Preethi and explore our laparoscopic solutions? Reach out to Marina’s Clinic for comprehensive care and personalised treatment plans. Contact us online or visit our clinic in Chennai to schedule an appointment. Recent Posts Everything You Want to Know About Hernias 12 Nov 2023 The Intricacies of Hashimoto's Disease: An In-Depth Look 12 Nov 2023 A Comprehensive Guide to Thyroid Symptoms and Solutions 12 Nov 2023 How to manage Hypothyroidism: The Crucial Role of Diet 12 Nov 2023 Importance Of Fibre In Our Diets 06 Nov 2023 Have Any Question? Contact us +91 98840 00171 [email protected]
9 Methods To Treat Acid Reflux Naturally
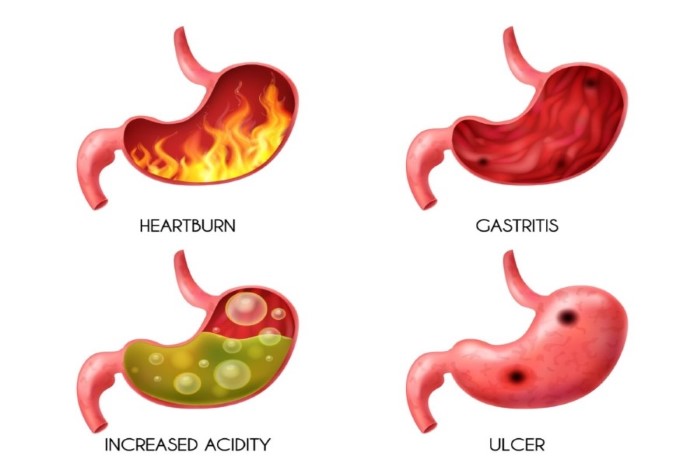
9 Methods To Treat Acid Reflux Naturally Before using medication to treat gastroesophageal reflux, it may be beneficial to make a few lifestyle changes. If you have a painful throat and a somewhat hoarse voice, you may be getting ready for the flu or a cold. However, if you’ve experienced these symptoms for some time, it’s possible that your lower esophageal sphincter, a valve, is to blame rather than a virus. That particular muscle regulates the opening between the oesophagus and the stomach, and if it doesn’t shut all the way, food and stomach acid can flow back into the oesophagus. Acid reflux is the backward flow of acid, and gastroesophageal reflux is the medical term for this ailment. You may get a bitter aftertaste in your mouth, sore throats, and hoarseness as a result of acid reflux. When acid reflux results in ongoing symptoms, it is referred to as gastroesophageal reflux disorder (GERD). Heartburn, which manifests as chest and upper abdominal pain, is the most typical symptom of GERD. Acid reflux is caused by three factors: inadequate stomach acid production, inadequate food or acid clearance from the oesophagus, and delayed stomach emptying. If you experience frequent heartburn or any other acid reflux symptoms, you might want to try the following advice given by our expert doctors at Marinas Clinic. Eat little and frequently: There may be greater reflux into the oesophagus when the stomach is really full. You might want to give “grazing,” or eating smaller meals more frequently rather than three meals a day, a try if it works with your schedule. Avoid certain foods: All except the blandest foods were traditionally advised to be avoided by those with acid reflux. But that’s not the case now. According to Dr. Preethi, our chief Surgeon at Marinas Clinic, “We’ve changed from the times when you couldn’t eat anything.” However, some foods continue to be more likely to cause reflux than others, such as mint, fatty meals, spicy foods, tomatoes, onions, and garlic, as well as coffee, tea, chocolate, and alcohol. If you routinely consume any of these items, you might try cutting them out to see if doing so reduces your reflux. If it does, you might then try bringing them back one at a time. A big NO for carbonated beverages: They cause burping, which opens the oesophagus to acid. Use still water in place of sparkling water. Keep awake after eating: While standing or even seated, gravity alone helps keep stomach acid where it belongs. Finish eating three hours before going to bed. This forbids snoozes in the afternoon, late supper, and midnight snacks. Don’t go too quickly: Avoid any vigorous activities for a few hours after eating. Walking after supper is acceptable, but strenuous exercise, especially if it involves bending over, can result in acid entering the oesophagus. Lie down inclined: Your head should be 6 to 8 inches higher than your feet in ideal circumstances.’Extra-tall’ bed risers can be used to achieve this by mounting them on the bed’s head support legs.. If your bed partner doesn’t like the change, think about using a foam wedge to support your upper body. Avoid attempting to construct a wedge by stacking cushions.Don’t attempt to stack pillows to form a wedge. They won’t provide you with the ongoing assistance you need. If instructed, reduce your weight: Gaining weight reduces the pressure that keeps the lower esophageal sphincter closed by dispersing the muscles that support it. Quit smoking if you do: The lower esophageal sphincter may relax as a result of nicotine. Examine your prescriptions: The sphincter can be relaxed by some medications, such as postmenopausal oestrogen, tricyclic antidepressants, and anti-inflammatory pain relievers, while the oesophagus can become irritated by others, particularly bisphosphonates like alendronate (Fosamax), ibandronate (Boniva), or risedronate (Actonel), which are used to increase bone density. As per our experts’ suggestion consult your doctor to rule out other causes if these measures don’t work or if you experience significant discomfort or trouble swallowing. Even if you make lifestyle modifications, reflux may still need to be treated with medication. Recent Posts Everything You Want to Know About Hernias 12 Nov 2023 The Intricacies of Hashimoto's Disease: An In-Depth Look 12 Nov 2023 A Comprehensive Guide to Thyroid Symptoms and Solutions 12 Nov 2023 How to manage Hypothyroidism: The Crucial Role of Diet 12 Nov 2023 Importance Of Fibre In Our Diets 06 Nov 2023 Have Any Question? Contact us +91 98840 00171 [email protected]
Everything You Should Know About Bariatric Surgery!
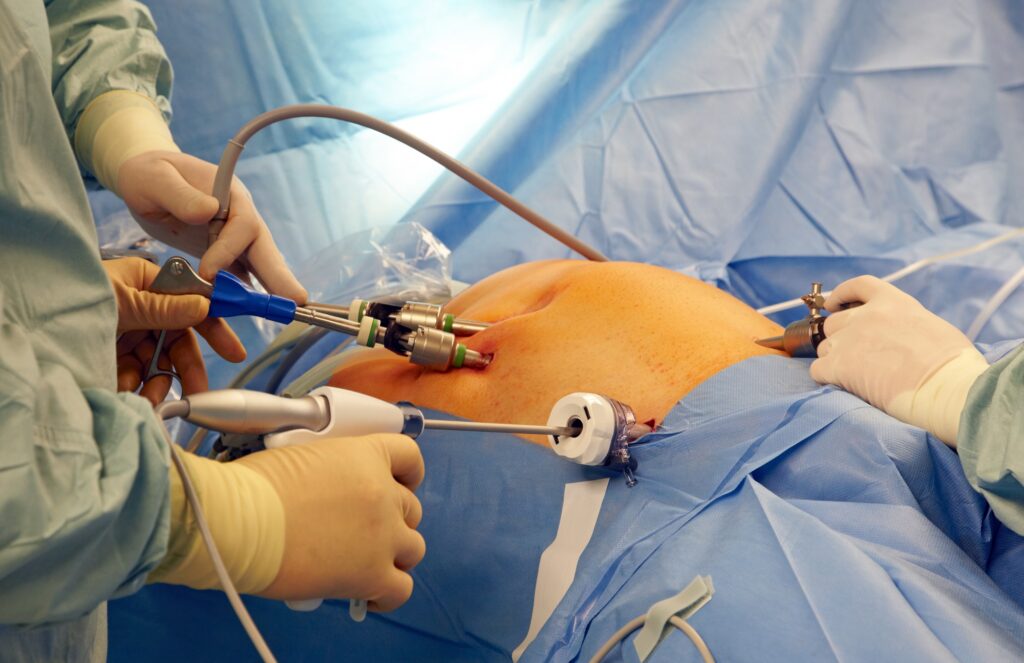
Everything You Should Know About Bariatric Surgery! People with extreme and excessive obesity are frequently unable to be properly treated with diet and exercise alone. Such people may undergo bariatric surgery as a procedure to assist them in losing weight. Evidence suggests that bariatric surgery, especially when combined with healthy diet and lifestyle modifications after surgery, may reduce death rates for people with severe obesity. By altering the digestive tract, bariatric surgery refers to surgical techniques that help patients lose weight. Gastric bypass and other weight loss surgeries, as well as other procedures, can all be referred to as “bariatric surgery.” Now let us know about BMI(Body Mass Index): In order to identify levels of obesity and evaluate whether bariatric intervention is necessary, the body mass index (BMI), a measurement of height in proportion to weight, is used. A BMI of over 40 kg/m2 or a BMI of over 35 kg/m2 in conjunction with serious health issues is referred to as clinically severe obesity. Type 2 diabetes, arthritis, heart disease, and severe obstructive sleep apnea are health issues connected to fat. The use of adjustable gastric bands is permitted by the Food and Drug Administration (FDA) for individuals with a BMI of 30 kg/m2 or more and at least one of these diseases. What are the principles of Bariatric Surgery: The main goals of bariatric surgery are to reduce food intake and intestinal and stomach absorption of nutrients. The mouth is where food is chewed and combined with saliva and other secretions that contain enzymes to begin the digestion process. Once the food is in the stomach, it is broken down and combined with digestive juices to allow the body to absorb the nutrients and calories. As food enters the duodenum, the first section of the small intestine, where it is combined with bile and pancreatic juice, digestion intensifies. The goal of bariatric surgery is to change or halt this digestive process so that food is not absorbed and broken down as usual. Patients can lose weight and lower their risk of obesity-related health hazards or diseases by consuming less calories and nutrients. Types of Bariatric Surgery: Depending on how much food the stomach can hold, how well the body can absorb nutrients, or a combination of the two, different consequences of bariatric surgery may be experienced. The most popular forms of bariatric surgery are the duodenal switch, adjustable gastric band, sleeve gastrectomy, and gastric bypass. Gastric Bypass: One of the most popular types of bariatric surgery is the gastric bypass procedure. The technique is divided into two steps, to put it simply. The top of the stomach is first separated from the other part of the stomach by a tiny pouch. When the first portion of the small intestine is split off, the bottom end is still connected to the newly developed little pouch in the stomach. The bottom of the small intestine is then joined to the top portion of the divided small intestine, which alters the food stream and results in alterations to gut hormones. This technique inhibits calorie and nutrient absorption as well as the amount of food the stomach can hold. Sleeve Gastrectomy: Involves cutting out about 80% of the stomach. What’s left is a sleeve, which is a tube-shaped pouch. The stomach can no longer hold as much food due to its reduced size. Additionally, it lessens the ghrelin hormone’s synthesis, which controls appetite. Gastric Band: An inflatable band is wrapped around the top of the stomach as part of the adjustable gastric band, resulting in a smaller pouch above. Patients feel full more quickly and less food can be stored. As improvements are made over time, the band gets smaller. Duodenal Switch: There are two elements to the Biliopancreatic Diversion with Duodenal Switch (BPD/DS). First, a tube-shaped pouch is made out of a part of the stomach (similar to sleeve gastrectomy). Second, the small intestine is largely bypassed. This limits the amount of food the stomach can hold and expedites the process of feeling full. The absorption of nutrients is also decreased. Although the procedure is very successful, there are higher risks, such as vitamin deficiency or starvation. Why Bariatric Surgery is Done: Having bariatric surgery can assist people who are extremely overweight lose weight and reduce their chance of developing serious, life-threatening health issues, including: Heart condition Stroke Elevated blood pressure Alcohol-unrelated fatty liver disease Slumber apnea Diabetes type 2 Conclusion: Keep in mind that not everyone who is overweight should undergo bariatric surgery. Medical requirements must be met. When other weight-loss methods, including changing your diet and exercising more, don’t work, it’s frequently advised.. At Marinas Clinic, the best bariatric surgeon is available to help you with the surgery.. Our team assists you in choosing the ideal course of action for every person based on their needs. We meticulously assess each patient before determining the kind of operation you require. Our experts choose wisely how to approach you and gives you the best chance for a successful weight loss. Recent Posts Everything You Want to Know About Hernias 12 Nov 2023 The Intricacies of Hashimoto's Disease: An In-Depth Look 12 Nov 2023 A Comprehensive Guide to Thyroid Symptoms and Solutions 12 Nov 2023 How to manage Hypothyroidism: The Crucial Role of Diet 12 Nov 2023 Importance Of Fibre In Our Diets 06 Nov 2023 Have Any Question? Contact us +91 98840 00171 [email protected]
Everything You Should Know About Laparoscopic Surgery
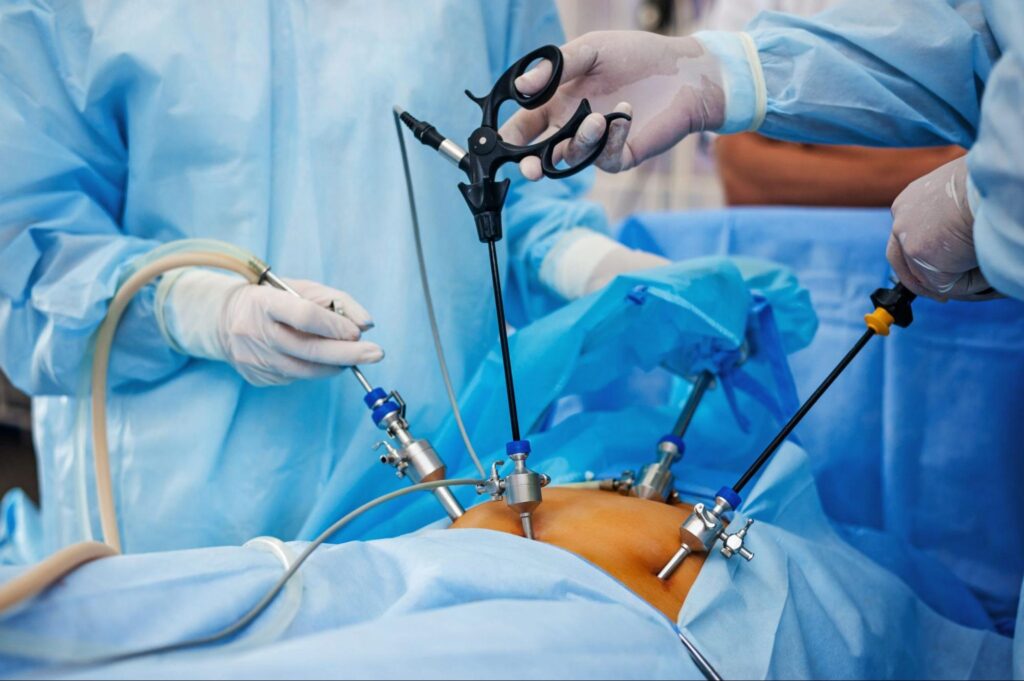
Everything You Should Know About Laparoscopic Surgery Surgeons have modified and mastered the skill of laparoscopic surgery over the past several years with the help of technology. Laparoscopic surgery is usually referred to as minimal invasive surgery or keyhole surgery. Laparoscopic surgery has become increasingly popular over time. Both therapeutic and exploratory purposes are often served by this method. Let’s learn more about the operation, its purpose, benefits, dangers, and other factors.What is Laparoscopic Surgery?Through tiny incisions, laparoscopic surgery enables doctors to look at or treat internal organs in the body. Recently, general surgeries, gynecological surgeries, and orthopedic operations have all employed this approach. Laparoscopic surgery uses a series of small cuts or incisions rather than a single large one as is required for conventional or open procedures.General anesthesia is used during laparoscopic procedures by a surgeon. Multiple 0.5–1 cm ports—incisions made by the surgeon—are then wont to implant trocars, which are tubular tools. The trocars are then employed by surgeons to insert a laparoscope and other specialist thin tools. A camera on the laparoscope transmits high-definition photos and films to a screen in the operating room. The opposite tools make cutting and mending easier, while the laparoscope directs the doctors across the operative area.What could also be done during a laparoscopic procedure?For the subsequent areas, laparoscopic or minimally invasive surgery is an efficient method:• Orthopedic surgery such as knee keyhole surgery or knee arthroscopy• Gallbladder surgery• Gynecological surgery like laparoscopic hysterectomy• Small and enormous intestine surgery• Hiatal hernia surgery• Appendix surgery• Liver, kidney, and pancreas surgery• Splenectomy• Laparoscopic infertility treatment• Gastroenterology surgery like gastric bypass• Colon and rectal surgery• Head and neck surgery• Cancer treatmentWhat advantages can laparoscopic procedures offer? Laparoscopic surgery provides certain benefits over conventional or open surgery. These consist of:• Smaller scars and incisions• A shorter stay within the hospital following surgery• More rapid recovery and healing• Less discomfort at the situation of the incision• Lessening the constraints placed on normal activities like driving and exercisingAre there any dangers with laparoscopic surgery? There are dangers related to all surgeries, invasive or keyhole. Among the complications are:• Infection at the location of surgery• Nausea and Vomiting• Damage to nearby arteries or organs• Sensitivity to anesthesia• Blood ClotsHow does laparoscopic surgery recovery look like? The patient moves into a hospital room or post-surgical room following surgery. The anesthetic frequently leaves the patient who is dazed and bewildered. Doctors and nurses monitor the patient’s vital signs and await any warning symptoms.The patient moves to a daily room as soon as they are awake and have the ability to eat, drink, and urinate. At this point , relatives of the patient may visit. The nurse gives instructions on washing, wound care, and post-operative care. Doctors advise using medications, particularly for constipation and pain control. Doctors also advise patients to not miss any follow-up sessions.Doctors can also suggest home post-surgical care services at this time for remote monitoring. These platforms also provide patients with access to worry coaches who are available around-the-clock, medical information, recovery-related reminders, nutritional, psychological, and physiotherapy help, among other things. The length of your time it takes to fully recover depends on the surgery, the patient’s health, and any problems. Laparoscopic diagnostic or exploratory operations may have up to five days for recovery. If one has minor laparoscopic surgery, like having their appendix removed, they will return to their normal activities after three weeks. Recovery from major laparoscopic surgery might take quite a year.How soon after surgery should a patient contact a doctor? If a patient has any of the symptoms listed below, they ought to get in touch with a doctor and ask for advice: Chillers and a heat Frequent vomiting Increase in abdomen pain, pain on one leg and swelling Pus and a nasty odor coming from the incision Pain and erythema at the surgery site The author of this text is Marinas Clinic, one of the best hospitals for Laparoscopic Surgeries. Connect with us for the best laparoscopic surgeon in Chennai and details on post-surgical care services following laparoscopic surgery. Recent Posts Everything You Want to Know About Hernias 12 Nov 2023 The Intricacies of Hashimoto's Disease: An In-Depth Look 12 Nov 2023 A Comprehensive Guide to Thyroid Symptoms and Solutions 12 Nov 2023 How to manage Hypothyroidism: The Crucial Role of Diet 12 Nov 2023 Importance Of Fibre In Our Diets 06 Nov 2023 Have Any Question? Contact us +91 98840 00171 [email protected]
What are the symptoms, Causes, and anal fissure treatment?

What are the symptoms, Causes, and anal fissure treatment? An anal fissure is a breach in the anus skin. It can affect people of various ages, although it is more frequent in children. In newborns and middle-aged adults, this is a reliable source. It is typically not a dangerous ailment, and the majority of individuals can cure it at home. However, reoccurring anal fissures or those that do not heal easily should be treated with caution. Continue reading to discover more about the causes of anal fissures and how to cure and avoid them in the future Symptoms One or more of the following symptoms may be caused by an anal fissure: • a noticeable rip in your anus skin• a noticeable rip in your anus skin a skin tag or tiny lump of skin close to the tear acute• discomfort in the anal region during bowel movements• traces of blood on stools or toilet paper after cleansing• anal region burning or itching Causes An anal fissure is most commonly caused by bypassing big or firm feces. Constipation or diarrhea regularly can potentially damage the skin surrounding your anus. However, not all anal fissures indicate a low-fiber diet or constipation. Poorly healed fissures or those situated in areas other than the posterior and midline of your anus might suggest an underlying disease. Other factors include: • squeezing or straining during birthing or bowel motions• having Crohn’s disease or another kind of inflammatory bowel disease (IBD).• a reduction in blood flow to the anorectal region• having anal sphincter muscles that are abnormally tight or spastic• taking part in anal sex• putting things into the anus Treatment Anal fissures usually heal in a few weeks if you take precautions to keep your stool soft, such as increasing your fiber and hydration intake. Bathing in warm water for 10 to 20 minutes many times each day, particularly after bowel motions, might help relax the sphincter and encourage healing. If your symptoms persist, you will most likely require more therapy. Nonsurgical therapies Your doctor may advise you to: – Nitroglycerin (Rectiv) was given externally to assist enhance blood flow to the fissure, facilitate healing, and relax the anal sphincter. When other conservative measures fail, nitroglycerin is often regarded as the medical therapy of choice. Headache, which might be severe, is one of the possible side effects. – Pain alleviation may be aided by topical anaesthetic creams such as lidocaine hydrochloride (Xylocaine). – Injection of botulinum toxin type A (Botox) to paralyse the anal sphincter muscle and ease spasms. – Oral nifedipine (Procardia) or diltiazem (Cardizem) can assist relax the anal sphincter. These drugs, which can be taken orally or administered topically, are used when nitroglycerin is ineffective or produces considerable negative effects. Surgery If you have a persistent anal fissure that has not responded to conventional therapies, or if your symptoms are severe, your doctor may advise surgery. Doctors typically conduct a treatment known as lateral internal sphincterotomy (LIS), which involves severing a tiny part of the anal sphincter muscle to relieve spasm and discomfort and encourage recovery. According to studies, surgery is far more beneficial than any medication therapy for persistent fissures. However, there is a slight chance that surgery will result in incontinence. Other Surgeries Menu HERNIA – INCISIONAL FISSURE LAPAROSCOPIC SURGEON APPENDICITIS THYROID GALL BLADDER STONES ACID REFLUX DIABETIC FOOT VARICOSE VEINS COLORECTAL SURGERY
3 signs you need to see a gastroenterologist in Chennai

Gastroenterologist in Chennai Gastroenterologist in Chennai To whom do you go if you have digestion and ulcer problems? A general practitioner. But would you still go to them if those problems are extreme? Well, this is where a gastroenterologist comes in. This doctor specializes in digestive related diseases. Digestion is a key part of our regular body function. Taking care of the GI system that controls the digestion of the food, absorbing nutrients, and excretion of the waste is important as much you pay attention to any part of your body. Our primary care doctor cannot treat if we face serious conditions in these areas and they direct you to a gastroenterologist who would diagnose the condition. 3 major signs you should turn to a gastroenterologist right away: Change in bowel habits Fewer bowel movements per week and prolonged diarrhoea should be checked as this may lead to serious health conditions.Constipation could also carry problems like hormonal malfunction, blockages, and even neurological issues. The longer you ignore the problem, the longer your health gets depleted. If you deal with this issue, check with a gastroenterologist as soon as possible. Rectal bleeding The apparent sign of rectal bleeding is blood on toilet paper or visible blood or red-tinged stool in the toilet bowl. However, you must pay attention to the color of the blood as it indicates different problems. Bright red blood indicates bleeding in the lower gastrointestinal tract. Dark red may indicate bleeding in the small intestine. Black and tarry stools may indicate bleeding from the upper part of the small intestine. Symptoms associated with rectal bleeding are fainting, feeling dizzy, rectal pain and abdominal pain. Recurring heartburn Frequent heartburn could be a sign of GERD (Gastroesophageal Reflux Disease). Reflux is a burning sensation that occurs behind the chest when stomach contents irritate the normal lining of the oesophagus and this may also lead to oesophageal cancer. If you’re over the age of 50, you should get a colon cancer screening. Men and women of this age have an increased risk of cancer symptoms. Never take the risk of ignoring these signs. You shouldn’t get embarrassed to get your symptoms checked. Get tested by a good gastroenterologist in Chennai and solve your problems. Though you place the trust in your primary care doctors, there are times it is mandatory to visit physicians who have spent their entire career developing an in-depth knowledge of gastrointestinal conditions. Stay healthy to stay happy. Recent Posts Importance Of Fibre In Our Diets 06 Nov 2023 Navigating Gut Health: Guide for Optimal Digestive Balance 06 Nov 2023 Endoscopy Explained: Procedure, Benefits, and Recovery 06 Nov 2023 The Impact of Stress on Gut Health: What You Need to Know 06 Nov 2023 Effective Approaches to Managing Chronic Acid Reflux 04 Nov 2023 Have Any Question? Contact us +91 98840 00171 [email protected]

