The Role of Mental Health in Managing Morbid Obesity

The Role of Mental Health in Managing Morbid Obesity Obesity is one of the most pressing health concerns of the modern world, affecting millions of individuals globally. Among the most severe forms of this condition is morbid obesity, which significantly elevates the risk of chronic illnesses such as diabetes, heart disease, and hypertension. While diet, exercise, and medical interventions play critical roles in managing this condition, the psychological aspect is often overlooked. Mental health is a vital component in managing morbid obesity, influencing not just eating habits but also the motivation and consistency required to sustain long-term weight management efforts.At Marinas Clinic in Chennai, renowned for its comprehensive approach to healthcare, Dr. Preethi Mrinalini, one of the best female surgeons in Chennai, emphasizes the importance of integrating mental health into obesity management. This holistic approach ensures that patients receive not only the necessary physical treatments but also the emotional and psychological support they need. The Link Between Mental Health and ObesityThere is a well-established connection between mental health and obesity. Studies have shown that individuals suffering from mental health disorders such as depression, anxiety, and stress are more likely to develop obesity. Emotional distress often leads to unhealthy eating behaviors, such as overeating or binge eating, as a way to cope with negative emotions. Conversely, people with obesity may experience low self-esteem, body image issues, and social isolation, leading to further mental health challenges.For those struggling with morbid obesity, the cycle can become even more vicious. The physical limitations imposed by severe obesity can exacerbate mental health struggles, making it more difficult to break free from unhealthy patterns. Therefore, addressing the mental and emotional well-being of individuals is essential for effective obesity management. Emotional Eating and Its ImpactOne of the most common psychological factors linked to obesity is emotional eating. Emotional eating refers to the consumption of food as a response to feelings rather than hunger. This behavior is particularly prevalent in individuals who struggle with anxiety, depression, or chronic stress. When faced with difficult emotions, individuals may turn to food as a way to soothe themselves, leading to weight gain over time.In many cases, people are not fully aware of the triggers behind their emotional eating. They may consume large quantities of high-calorie, sugary, or fatty foods when they feel sad, lonely, or bored. Identifying these triggers and developing healthier coping mechanisms is crucial for successful weight management. Cognitive-behavioral therapy (CBT) and mindfulness-based interventions are often recommended as part of a comprehensive treatment plan for individuals struggling with emotional eating. The Role of Therapy in Weight ManagementFor individuals with morbid obesity, traditional weight loss strategies like diet and exercise are often not enough. This is where therapy can play a transformative role. Cognitive-behavioral therapy (CBT) helps individuals identify and change the negative thought patterns and behaviors that contribute to overeating. It also teaches patients how to develop healthier ways to cope with stress, anxiety, and other emotional triggers. Psychotherapy can also address underlying issues that contribute to obesity, such as trauma, grief, or unresolved emotional conflicts. By resolving these issues, patients can gain a better understanding of their relationship with food and develop a more positive body image. Support groups, whether in person or online, can provide additional emotional support for individuals facing the challenges of morbid obesity. Knowing that they are not alone in their journey can significantly boost their motivation and sense of accountability. Managing Stress for Better Health OutcomesStress is a significant contributing factor to weight gain, particularly in individuals with morbid obesity. Chronic stress triggers the release of cortisol, a hormone that promotes fat storage, especially around the abdomen. Additionally, stress often leads to poor sleep, which further disrupts the body’s hormonal balance and increases appetite.Mindfulness practices, such as meditation and deep breathing exercises, can be effective in managing stress and reducing emotional eating. These practices help individuals become more aware of their emotions and bodily sensations, allowing them to respond to stress in a healthier manner. By incorporating mindfulness into a weight management plan, individuals can better regulate their emotional responses and make more conscious decisions about their eating habits. The Importance of Self-CompassionMorbid obesity can be an isolating and emotionally taxing condition. Individuals struggling with their weight often face societal stigma, which can exacerbate feelings of shame and guilt. This negative self-perception can hinder progress in weight management, making it even more difficult for individuals to stick to their health goals.Practicing self-compassion is essential for long-term success. By learning to treat themselves with kindness and understanding, individuals can break the cycle of negative self-talk and adopt a more positive outlook on their weight loss journey. Self-compassion helps individuals stay motivated, even when they experience setbacks, and promotes a healthier, more balanced relationship with their bodies. ConclusionAddressing mental health is key to effectively managing morbid obesity. The journey to weight loss and better health requires more than just physical interventions—it involves overcoming psychological hurdles and developing emotional resilience. At Marinas Clinic, Dr. Preethi Mrinalini, a leading surgeon in Chennai, advocates for a holistic approach to obesity management, one that integrates mental health support alongside medical treatments. By prioritizing both the mind and body, individuals struggling with morbid obesity can achieve lasting, transformative results. Recent Posts The Impact of Morbid Obesity on Daily Life: Real-Life Experiences 21 Oct 2024 The Role of Mental Health in Managing Morbid Obesity 21 Oct 2024 What to Expect in the First Month After Your Weight Loss Surgery 14 Oct 2024 Expert Tips for Eating Well After Weight Loss Surgery 14 Oct 2024 Preparing for Your First Consultation: Questions to Ask About Varicose Vein Treatment Options 07 Oct 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
What to Expect in the First Month After Your Weight Loss Surgery

What to Expect in the First Month After Your Weight Loss Surgery What to Expect in the First Month After Your Weight Loss SurgeryWeight loss surgery, also known as bariatric surgery, can be a life-changing procedure that helps individuals achieve significant weight loss and improve overall health. However, the journey doesn’t end once the surgery is completed. The first month after your surgery is a crucial period of adjustment, where your body heals and adapts to new dietary and lifestyle habits. Understanding what to expect during this time can help ease any anxiety and ensure a smoother recovery process. Under the expertise of Dr. Preethi Mrinalini, one of the best female surgeons in Chennai, and her team at Marinas Clinic, patients are guided through every stage of their recovery with care and support. If you are considering weight loss surgery or have just undergone the procedure, here’s what to expect in the first month after surgery. Week 1: Recovery and RestThe first week following weight loss surgery is primarily about rest and recovery. Since the procedure is typically done laparoscopically, the incisions made are small, and healing time is generally quicker compared to open surgeries. However, you may still experience soreness, fatigue, and discomfort around the surgical area. During this initial recovery phase, your doctor will advise you to avoid strenuous activities. Walking, however, is encouraged to help prevent blood clots and promote circulation. Simple movements like walking around the house every few hours will aid in your recovery and prevent stiffness. Your diet during the first week will be strictly liquid-based. This helps your stomach heal without being strained. Clear broths, sugar-free drinks, and protein shakes are common components of this phase. Hydration is key, but you’ll need to sip liquids slowly to avoid overloading your stomach. Week 2: Moving to Soft FoodsAs you enter the second week post-surgery, your doctor may give you the green light to transition from a liquid diet to soft, pureed foods. These may include protein-rich items like Greek yogurt, scrambled eggs, or well-pureed vegetables. You’ll also continue with protein shakes to ensure you are meeting your nutritional needs. It’s essential to remember that your stomach will still be adjusting. Eating too much or too quickly can cause nausea, discomfort, or vomiting. Be sure to eat very small amounts, chew food thoroughly, and listen to your body’s cues of fullness. This week, you’ll also gradually begin to feel stronger. While walking will still be your main form of physical activity, you might start to increase your movement slightly. However, avoid heavy lifting or anything that strains your core muscles. Week 3: Adjusting to a New RoutineBy the third week, most patients start to feel a sense of normalcy return, but the adjustment period continues. You’ll likely be able to eat slightly more solid foods in small portions, but focus should remain on soft, easy-to-digest options. Proteins such as soft-cooked fish or finely ground meats might be introduced. Staying hydrated remains a priority, and it’s important to keep sipping water throughout the day. However, avoid drinking liquids with meals, as this can lead to feeling overly full too quickly. At this stage, many patients start noticing the first significant drops in weight. While this can be exciting, it’s essential to follow the doctor’s nutritional advice carefully to ensure the weight loss is steady and healthy. Incorporating light physical activities, such as short walks or gentle stretching exercises, can help your body adjust to the weight loss process. Week 4: Progressing with Solid Foods and Light ActivityBy the end of the first month, many patients will have progressed to eating more solid foods, but the focus should remain on healthy, nutrient-dense options. Your meals should be small, protein-focused, and spread out throughout the day. Protein intake is critical, as it helps with muscle maintenance during rapid weight loss. Ensure you’re including lean proteins like chicken, turkey, or tofu. While your energy levels will likely improve during this week, it’s still important to avoid any intense physical activities. You can start incorporating low-impact exercises such as walking longer distances, swimming, or cycling, but always consult your surgeon before starting any new exercise regime. Patients often experience a variety of emotional changes during this time as well. Weight loss surgery can be an emotional journey, and it’s not uncommon to feel overwhelmed, excited, or even anxious about the changes you’re experiencing. Surrounding yourself with support, whether it’s from your family, friends, or a support group, can help you stay motivated and emotionally balanced. Conclusion: The First Step in a Lifelong JourneyThe first month after weight loss surgery is a period of significant physical and emotional adjustments. While the early stages might be challenging, the long-term benefits of the surgery—improved health, greater mobility, and enhanced quality of life—make the effort worthwhile. With the guidance of Dr. Preethi Mrinalini, a renowned surgeon in Chennai, and the team at Marinas Clinic, you can feel confident knowing that you are in expert hands throughout this transformative process. Always remember that weight loss surgery is not a quick fix but the beginning of a lifelong commitment to healthier habits. Following your doctor’s instructions carefully, staying mindful of your new eating patterns, and maintaining an active lifestyle will set you on the path to sustained success. Recent Posts What to Expect in the First Month After Your Weight Loss Surgery 14 Oct 2024 Expert Tips for Eating Well After Weight Loss Surgery 14 Oct 2024 Preparing for Your First Consultation: Questions to Ask About Varicose Vein Treatment Options 07 Oct 2024 The Impact of Pregnancy on Varicose Veins: A Guide for Expecting Mothers 07 Oct 2024 The Link Between Diabetes and Foot Ulcers: Prevention and Treatment Options 30 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
Expert Tips for Eating Well After Weight Loss Surgery

Expert Tips for Eating Well After Weight Loss Surgery Weight loss surgery, also known as bariatric surgery, can be a life-changing step for many individuals who are battling obesity. While the surgery itself is a significant milestone, the journey to a healthier you doesn’t end there. Post-surgery, your eating habits will require thoughtful changes to ensure optimal results and long-term success. Adopting the right dietary habits can help you heal faster, maintain your weight loss, and lead a healthier life. Dr. Preethi Mrinalini, a highly regarded surgeon at Marinas Clinic, shares expert tips on how to eat well after weight loss surgery. 1. Understand Your New StomachWeight loss surgeries, such as gastric bypass or sleeve gastrectomy, significantly reduce the size of your stomach. This means your stomach can hold far less food than it used to, and overeating can lead to discomfort, nausea, and even complications. Immediately after surgery, your diet will transition from liquids to soft foods and eventually solid foods. Understanding this gradual progression is key. Early on, stick to liquids and purees as instructed by your healthcare provider, and slowly work your way to more solid foods over several weeks. 2. Small Portions are KeyAfter weight loss surgery, you will need to adjust to eating smaller portions. It’s important to eat mindfully and listen to your body’s hunger cues. Meals that were once normal-sized may now seem far too large, and that’s completely fine. Eating smaller, more frequent meals throughout the day will help you stay satisfied and energized without overwhelming your stomach. Aim for 4-6 small meals daily, and remember to stop eating as soon as you feel full to avoid any strain on your digestive system. 3. Protein Should Be Your PriorityProtein is the most important nutrient after weight loss surgery. It helps with tissue healing, maintaining muscle mass, and keeping you feeling full for longer. Since your stomach’s capacity is limited, prioritize protein at every meal. Include lean protein sources like chicken, turkey, fish, eggs, and tofu. If you have trouble getting enough protein from whole foods, consider protein supplements as recommended by your healthcare team. 4. Stay Hydrated, but Time It RightStaying hydrated is crucial, especially after weight loss surgery, as dehydration can become a common issue. However, you should avoid drinking fluids during meals. Drinking while eating can fill your small stomach too quickly and leave little room for food, which can lead to discomfort or malnutrition. Instead, drink fluids between meals—at least 30 minutes before or after eating. Aim for at least 64 ounces of water per day, but remember to sip slowly to avoid overwhelming your stomach. 5. Chew Slowly and ThoroughlyAfter surgery, food needs to be broken down thoroughly before it reaches your stomach. Chewing slowly and completely helps prevent blockages, nausea, and discomfort. Take smaller bites and chew each bite at least 20-30 times before swallowing. Eating slowly also helps you recognize when you’re full, which can prevent overeating and ensure proper digestion. 6. Avoid Sugary and Fatty FoodsSugary and fatty foods can cause digestive issues after weight loss surgery, particularly a condition known as dumping syndrome. This occurs when food moves too quickly from your stomach to your small intestine, causing symptoms like nausea, vomiting, and diarrhea. Avoid sweets, sugary drinks, fried foods, and high-fat snacks. Instead, choose nutrient-dense options that provide the vitamins and minerals your body needs to stay healthy and energized. 7. Incorporate Vitamins and SupplementsSince weight loss surgery can limit your body’s ability to absorb certain nutrients, it’s essential to take vitamins and supplements as recommended by your doctor. Common deficiencies after surgery include vitamin B12, iron, calcium, and vitamin D. Taking a daily multivitamin and any additional supplements prescribed by your healthcare provider will help prevent deficiencies and ensure that you’re getting the nutrients your body needs to thrive. 8. Maintain a Food JournalKeeping track of what you eat can help you stay on top of your nutritional goals and monitor any patterns or issues that arise. A food journal can also help you communicate more effectively with your healthcare team if you experience any digestive issues or weight plateaus. Documenting your meals, portion sizes, and how you feel after eating can give you valuable insights into your eating habits and ensure you’re on the right track. 9. Follow-Up Care is EssentialRegular follow-up appointments with your healthcare team are vital for tracking your progress and addressing any concerns. Your surgeon and nutritionist will help monitor your weight loss, nutritional intake, and overall health. Make sure to attend all scheduled appointments and discuss any challenges you may be facing with your diet or lifestyle. They can offer valuable advice and adjustments to keep you moving toward your goals. ConclusionEating well after weight loss surgery is a long-term commitment that requires thoughtful planning and dedication. By following these expert tips, you can maintain your weight loss, support your health, and enjoy a better quality of life. Dr. Preethi Mrinalini, one of the best female surgeons in Chennai, emphasizes that understanding your body’s new needs and making informed food choices is key to lasting success. With the right approach, you can enjoy a healthy, balanced diet and thrive after your surgery. Recent Posts What to Expect in the First Month After Your Weight Loss Surgery 14 Oct 2024 Expert Tips for Eating Well After Weight Loss Surgery 14 Oct 2024 Preparing for Your First Consultation: Questions to Ask About Varicose Vein Treatment Options 07 Oct 2024 The Impact of Pregnancy on Varicose Veins: A Guide for Expecting Mothers 07 Oct 2024 The Link Between Diabetes and Foot Ulcers: Prevention and Treatment Options 30 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
The Link Between Diabetes and Foot Ulcers: Prevention and Treatment Options

The Link Between Diabetes and Foot Ulcers: Prevention and Treatment Options Diabetes is a growing health concern that affects millions worldwide. While managing blood sugar levels is the primary focus of treatment, diabetes can lead to several complications if not well controlled. One such complication is diabetic foot ulcers, a condition that often goes unnoticed until it becomes severe. Understanding the link between diabetes and foot ulcers, along with how to prevent and treat this issue, is crucial for every diabetic patient.Dr. Preethi Mrinalini, a renowned consultant surgeon at Marinas Clinic and Apollo Hospitals, emphasizes the importance of early detection and proper management of diabetic foot ulcers. With years of experience as one of the best female surgeons in Chennai, she sheds light on how individuals with diabetes can protect their feet from ulcers and other related complications.How Does Diabetes Cause Foot Ulcers?Diabetes affects the body in several ways, but its impact on circulation and nerve function is directly linked to foot ulcers. High blood sugar levels can damage blood vessels, leading to poor circulation, particularly in the lower extremities. This reduced blood flow makes it harder for the body to heal minor injuries such as cuts, blisters, or sores. Additionally, diabetes can cause nerve damage, a condition known as diabetic neuropathy, which dulls the sensation in the feet.People with diabetic neuropathy might not feel pain when they injure their foot, allowing minor issues to worsen over time. A small blister, when left untreated, can become infected and develop into a serious ulcer.Risk Factors for Diabetic Foot UlcersSome diabetic patients are more prone to foot ulcers than others. The following risk factors can increase the likelihood of developing foot ulcers: Poorly managed blood sugar: Uncontrolled diabetes can lead to faster nerve damage and circulation issues, making it harder for the body to heal injuries. Peripheral artery disease (PAD): PAD reduces blood flow to the extremities, further increasing the risk of foot ulcers. Foot deformities: Conditions such as bunions, hammertoes, and flat feet can cause pressure points that lead to ulcers. Improper footwear: Wearing shoes that are too tight or uncomfortable can cause blisters or sores, which can develop into ulcers. Smoking: Smoking constricts blood vessels and reduces circulation, which can slow down the healing process. History of foot ulcers: If you’ve had a foot ulcer in the past, you are more likely to develop another. Prevention of Diabetic Foot UlcersPreventing foot ulcers requires a proactive approach. Diabetic patients should take extra care of their feet and adopt preventive measures, including: Regular Foot Inspections: Examine your feet daily for any cuts, blisters, redness, or swelling. Using a mirror can help you see areas that are difficult to reach. Proper Footwear: Always wear well-fitting shoes that provide support and cushioning. Special diabetic shoes are available to reduce pressure points on the feet. Keep Feet Clean and Moisturized: Clean your feet daily with lukewarm water, dry them thoroughly, and apply moisturizer to prevent dry skin, which can crack and lead to infections. Regular Medical Checkups: Regular visits to your healthcare provider for foot exams can help detect any issues early. Your doctor may recommend seeing a podiatrist for specialized foot care. Control Blood Sugar Levels: Managing your diabetes effectively is the most critical preventive measure. Keeping your blood sugar within the target range can help reduce nerve and blood vessel damage. Treatment Options for Diabetic Foot UlcersIf a foot ulcer develops, early intervention is essential to prevent complications such as infection or the need for amputation. Treatment options vary based on the severity of the ulcer: Wound Care: Proper cleaning and dressing of the wound are crucial. Your healthcare provider may remove dead tissue (debridement) to promote healing. Offloading: Reducing pressure on the affected foot is important for recovery. This can be done with specialized footwear, crutches, or a wheelchair in severe cases. Medications: Antibiotics may be prescribed if the ulcer is infected. In some cases, your doctor may recommend medications that promote healing by improving circulation. Surgical Intervention: For ulcers that do not respond to conservative treatment, surgery may be required. Surgical options include correcting foot deformities or improving blood flow through vascular surgery. Advanced Therapies: Hyperbaric oxygen therapy and growth factor treatments are some of the advanced therapies available for stubborn foot ulcers. When to See a DoctorIt’s essential for diabetic patients to seek medical attention as soon as they notice any signs of foot ulcers. Delaying treatment can lead to infections, which may result in severe complications, including amputation.At Marinas Clinic, Dr. Preethi Mrinalini provides comprehensive care for diabetic foot ulcers, helping patients manage their condition with the latest medical techniques. As the best female surgeon in Chennai, she advocates for a multidisciplinary approach, combining wound care, medication, and lifestyle adjustments to ensure the best outcomes.ConclusionDiabetic foot ulcers are a serious but preventable complication of diabetes. With proper foot care, regular checkups, and effective diabetes management, individuals can significantly reduce their risk of developing ulcers. However, if a foot ulcer does occur, early treatment is essential to prevent complications. Consulting with experts like Dr. Preethi Mrinalini at Marinas Clinic ensures that you receive the best possible care, tailored to your needs. Recent Posts The Link Between Diabetes and Foot Ulcers: Prevention and Treatment Options 30 Sep 2024 Common Myths About Diabetic Foot Care Debunked 30 Sep 2024 The Psychological Impact of Ovarian Cysts: Coping Strategies and Support Resources 23 Sep 2024 How to Prepare for Your Doctor’s Appointment Regarding Ovarian Cysts 23 Sep 2024 How to Prevent Diabetic Foot Complications: Practical Tips from Experts 16 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
Common Myths About Diabetic Foot Care Debunked

Common Myths About Diabetic Foot Care Debunked Diabetes is a chronic condition that affects millions of people worldwide, and one of its most significant complications is foot-related problems. Diabetic foot issues, ranging from ulcers to infections, can lead to severe consequences if left untreated. Yet, misconceptions surrounding diabetic foot care often hinder proper management, putting individuals at risk. In this blog, we will debunk some of the most common myths about diabetic foot care and highlight the importance of regular medical checkups.Dr. Preethi Mrinalini, a renowned surgeon at Marinas Clinic and widely regarded as the best female surgeon in Chennai, emphasizes the critical role of accurate information in managing diabetic foot conditions. Patients often fall prey to myths and false beliefs that can delay treatment and worsen the condition. With expert insights, let’s explore and debunk some common myths about diabetic foot care.Myth 1: “If My Feet Feel Fine, I Don’t Need to Worry”Many people believe that if they aren’t experiencing any pain or discomfort in their feet, they don’t need to worry about complications. This is a dangerous misconception. Diabetes can cause nerve damage, also known as diabetic neuropathy, which reduces sensation in the feet. You may not feel pain even if there’s an injury, blister, or infection developing.Truth: Regular foot exams are crucial for all diabetics, even if you don’t experience any symptoms. Early detection of wounds, changes in skin color, or foot deformities can prevent complications like ulcers or amputations.Myth 2: “Home Remedies Are Enough to Treat Diabetic Foot Issues”Some people with diabetes rely on home remedies, such as applying lotions, herbal treatments, or soaking their feet in warm water, believing that these methods can heal or prevent foot issues. While self-care is important, it’s a mistake to assume that home remedies alone can manage diabetic foot conditions.Truth: Proper diabetic foot care involves more than home remedies. Professional medical advice is essential to ensure that even minor issues are promptly addressed. If left untreated, small wounds can quickly escalate into serious infections. Always consult with a healthcare professional, especially if you notice cuts, blisters, or infections.Myth 3: “I Don’t Need to Worry About Shoes”Footwear might seem like a trivial concern, but for people with diabetes, wearing the wrong shoes can lead to serious issues. Some believe that any comfortable shoe is good enough, not realizing that specific features, such as proper fit and cushioning, are vital to protecting their feet.Truth: Diabetic patients should invest in shoes designed specifically for people with diabetes, as these shoes provide extra cushioning and minimize the risk of friction or pressure that can lead to foot injuries. Custom orthotics or specialized diabetic shoes can make a significant difference in preventing foot problems.Myth 4: “Minor Foot Issues Will Heal on Their Own”Some diabetics believe that minor foot injuries, such as small cuts or blisters, will heal naturally over time. While this might be true for people without diabetes, it’s not the case for those with this condition. Diabetes often impairs blood circulation, which can slow the healing process, leading to prolonged and severe infections.Truth: Even minor foot problems can escalate into serious complications for diabetics. Regular monitoring and immediate treatment of any wound, no matter how small, is essential to prevent infections that could require more invasive treatment, such as surgery.Myth 5: “If I Don’t Have High Blood Sugar, I’m Safe from Foot Problems”Another common belief is that diabetic foot problems are only associated with poorly controlled blood sugar levels. While high blood sugar does increase the risk of complications, even those with well-managed diabetes can face foot issues due to neuropathy or poor circulation.Truth: Neuropathy and circulation issues can occur even in diabetics who maintain good blood sugar control. It’s vital to monitor your feet regularly, regardless of how well-controlled your blood sugar levels are. Maintaining good foot hygiene and attending regular foot checkups are necessary preventive measures.Myth 6: “I Only Need to See a Doctor if There’s a Problem”This is one of the most dangerous myths regarding diabetic foot care. Many patients avoid visiting a doctor unless they notice a visible or painful issue with their feet. However, diabetic foot problems can develop slowly, and by the time symptoms appear, the condition may have progressed significantly.Truth: Preventive care is key. Regular checkups with a foot care specialist can detect problems before they become serious. Diabetics should make foot care a part of their routine health checkups, even if they aren’t experiencing any noticeable issues.ConclusionDebunking these common myths about diabetic foot care is crucial for managing the condition effectively and preventing severe complications. It’s essential for diabetics to understand the importance of regular checkups, proper footwear, and immediate attention to even minor foot issues.At Marinas Clinic, Dr. Preethi Mrinalini, widely recognized as the best female surgeon in Chennai, provides expert care and guidance for managing diabetic foot complications. Regular consultations with a specialist can significantly improve outcomes and ensure that foot health is maintained effectively.If you or a loved one has diabetes, don’t let these myths put your foot health at risk. Always consult with your healthcare provider to get the proper care and advice tailored to your condition. Recent Posts The Link Between Diabetes and Foot Ulcers: Prevention and Treatment Options 30 Sep 2024 Common Myths About Diabetic Foot Care Debunked 30 Sep 2024 The Psychological Impact of Ovarian Cysts: Coping Strategies and Support Resources 23 Sep 2024 How to Prepare for Your Doctor’s Appointment Regarding Ovarian Cysts 23 Sep 2024 How to Prevent Diabetic Foot Complications: Practical Tips from Experts 16 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
The Psychological Impact of Ovarian Cysts: Coping Strategies and Support Resources
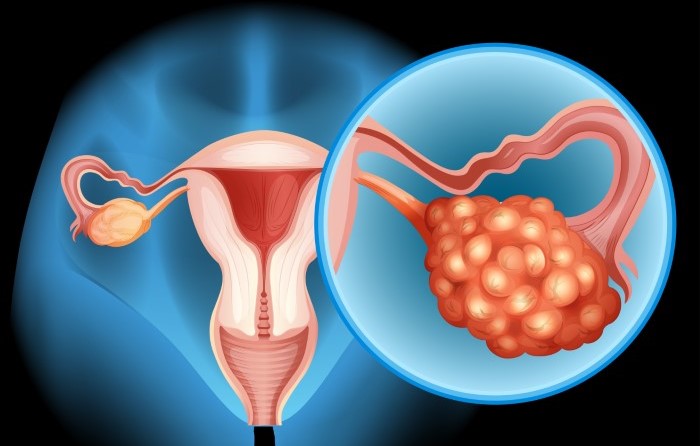
The Psychological Impact of Ovarian Cysts: Coping Strategies and Support Resources Ovarian cysts are a common gynecological issue that affect many women at some point in their lives. While often benign and asymptomatic, ovarian cysts can sometimes lead to physical discomfort, emotional distress, and psychological challenges. This blog will explore the psychological impact of ovarian cysts and offer coping strategies and support resources for women facing this condition. Understanding and addressing these emotional aspects is essential in fostering both mental and physical well-being.At Marinas Clinic in Chennai, Dr. Preethi Mrinalini, a highly respected surgeon, is committed to providing comprehensive care to women dealing with ovarian cysts. As one of the best female surgeons in Chennai, Dr. Preethi focuses on not only treating the physical symptoms but also guiding patients through the emotional and psychological complexities of their condition. Understanding the Psychological Impact of Ovarian CystsFor many women, the discovery of an ovarian cyst can trigger feelings of anxiety and fear. The word “cyst” itself can evoke concerns about potential malignancy, even though most ovarian cysts are benign. Women may also experience a range of emotions, including: Fear of the Unknown: The initial diagnosis of an ovarian cyst often leads to fear of complications such as ovarian cancer, infertility, or the need for surgery. The uncertainty surrounding the condition can heighten feelings of stress and anxiety. Body Image Concerns: Women may feel self-conscious or distressed about changes in their body, especially if the cyst leads to bloating, weight fluctuations, or discomfort. These physical changes can negatively affect self-esteem and body image. Emotional Exhaustion: Chronic pain or discomfort from cysts can wear down a person’s emotional resilience. Constant discomfort, fatigue, and managing doctor’s appointments or treatments can contribute to emotional exhaustion, which may lead to feelings of frustration, irritability, or even depression. Social Isolation: Women suffering from ovarian cysts may avoid social events or withdraw from activities due to pain or anxiety about their condition. This isolation can further exacerbate feelings of loneliness and sadness. Coping Strategies for Dealing with Ovarian CystsManaging the emotional challenges of ovarian cysts is crucial for overall health. Here are some coping strategies that can help women deal with the psychological impact of their condition: Educate Yourself: Understanding your diagnosis is one of the most effective ways to combat fear and uncertainty. Speak to your healthcare provider, ask questions, and research reliable sources about ovarian cysts. Learning more about the condition will help you feel more in control and reduce anxiety. Practice Mindfulness and Relaxation Techniques: Stress can exacerbate symptoms and affect your emotional well-being. Practices such as deep breathing, meditation, and yoga can help calm your mind, reduce anxiety, and enhance your ability to cope with stress. Seek Emotional Support: Sharing your feelings with trusted friends, family, or a support group can significantly ease the emotional burden. Whether it’s venting your frustrations or receiving reassurance, emotional support can reduce feelings of isolation and helplessness. Focus on Your Physical Health: Regular exercise, a balanced diet, and adequate sleep can help manage some of the physical symptoms associated with ovarian cysts. Physical well-being often contributes to improved mental well-being, creating a positive cycle of care. Cognitive Behavioral Therapy (CBT): If anxiety, depression, or negative thought patterns become overwhelming, cognitive behavioral therapy (CBT) can be an effective treatment. CBT focuses on identifying and changing negative thoughts and behaviors, helping women regain control over their emotional health. Consult with a Specialist: In some cases, speaking with a mental health professional, such as a psychologist or counselor, can be beneficial. Professional counseling provides a safe space to discuss fears, anxiety, and emotional stress associated with the condition. Support Resources for Women with Ovarian CystsWomen facing the psychological impact of ovarian cysts have several resources at their disposal to seek help and support: Online Support Communities: There are numerous online forums and social media groups where women can share their experiences, offer advice, and support one another. Websites such as the Ovarian Cancer Research Alliance (OCRA) or community boards like Reddit’s women’s health section provide spaces for discussion and connection. Local Support Groups: Many hospitals and clinics offer support groups for women dealing with reproductive health issues. These groups can be an excellent resource for sharing personal experiences and learning from others in a similar situation. Counseling Services: If you feel that your emotional distress is impacting your daily life, seeking help from a licensed counselor or psychologist can provide relief. Mental health professionals can offer coping strategies tailored to your needs and assist in managing anxiety, depression, or emotional exhaustion. Educational Resources: Websites such as Mayo Clinic, WebMD, and specialized health organizations offer comprehensive information about ovarian cysts, treatment options, and emotional support strategies. Educating yourself through reliable resources will help in managing your health and emotional well-being. ConclusionThe emotional and psychological toll of ovarian cysts can be significant, but with the right coping strategies and support, women can navigate these challenges effectively. Seeking support from loved ones, accessing professional mental health services, and staying informed about the condition can make a tremendous difference in managing the emotional effects of ovarian cysts.At Marinas Clinic, Dr. Preethi Mrinalini, one of the best female surgeons in Chennai, is dedicated to ensuring that her patients receive holistic care, addressing both their physical and emotional needs. With expert guidance and the right resources, women can regain control over their health and well-being while managing ovarian cysts. Recent Posts The Psychological Impact of Ovarian Cysts: Coping Strategies and Support Resources 23 Sep 2024 How to Prepare for Your Doctor’s Appointment Regarding Ovarian Cysts 23 Sep 2024 How to Prevent Diabetic Foot Complications: Practical Tips from Experts 16 Sep 2024 Yoga and Haemorrhoids: Poses That Can Help Relieve Symptoms 16 Sep 2024 Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai 10 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
How to Prepare for Your Doctor’s Appointment Regarding Ovarian Cysts
How to Prepare for Your Doctor’s Appointment Regarding Ovarian Cysts When it comes to health concerns like ovarian cysts, preparing for a doctor’s appointment can feel overwhelming. Ovarian cysts, which are fluid-filled sacs that develop on or inside the ovaries, are common among women, often presenting no symptoms. However, for some, they can cause discomfort, pain, or other complications. If you’ve been diagnosed with an ovarian cyst or are concerned about symptoms, it’s important to make the most of your doctor’s appointment by being well-prepared.At Marinas Clinic in Chennai, you’ll find some of the best medical professionals to guide you through the process, including Dr. Preethi Mrinalini, widely regarded as one of the best female surgeons in Chennai. This guide will help you understand how to prepare for your appointment, ensuring you can approach it with confidence and peace of mind. 1. Understand Your SymptomsBefore you visit your doctor, take the time to understand your symptoms and how they impact your daily life. This can include things like: Pelvic pain or pressure Bloating Irregular periods Pain during intercourse or bowel movements Unexplained weight gain Keep a journal of your symptoms, noting when they started, how often they occur, and whether they coincide with your menstrual cycle. This will give your doctor valuable insight into your condition and help them recommend the right course of action. 2. Know Your Medical HistoryYour doctor will need a complete overview of your medical history to assess your risk for ovarian cysts. Make sure you can provide details on the following:Previous surgeries or medical conditionsAny history of ovarian cysts or other reproductive issuesYour menstrual history, including the regularity and duration of your periodsAny hormonal treatments or medications you’ve takenA family history of reproductive health issues or cancersBeing prepared with this information will help your doctor determine whether further tests or treatments are necessary. 3. Prepare a List of QuestionsOvarian cysts can be a complex issue, and it’s natural to have questions. Before your appointment, prepare a list of questions you’d like to ask your doctor. These might include:What type of ovarian cyst do I have?Is the cyst likely to go away on its own?What treatment options are available?Could this cyst affect my fertility or future pregnancies?What symptoms should I watch out for that might indicate a complication?Asking the right questions will give you a clearer understanding of your condition and what to expect moving forward. 4. Bring a List of Current MedicationsDuring your appointment, your doctor will need to know about any medications or supplements you’re currently taking. This includes: Prescription medications Over-the-counter drugs Herbal supplements or vitamins Providing a comprehensive list will help your doctor understand how your current treatments may interact with potential treatments for ovarian cysts. 5. Be Ready for Diagnostic TestsDepending on your symptoms and medical history, your doctor may recommend certain diagnostic tests during your appointment. These could include: Ultrasound: A pelvic ultrasound is the most common imaging test used to detect and evaluate ovarian cysts. Blood tests: If your doctor suspects that your cyst may be cancerous, they may recommend blood tests like the CA-125 test, which can help detect ovarian cancer. Laparoscopy: In some cases, especially if the cyst is causing severe symptoms or is suspected to be cancerous, your doctor may suggest a minimally invasive surgical procedure called a laparoscopy. Understanding the potential tests beforehand will help reduce any anxiety and allow you to ask informed questions during your appointment. 6. Consider Bringing a Support PersonIt’s normal to feel anxious about discussing health issues with your doctor. Consider bringing a trusted friend or family member to your appointment. They can help take notes, ask questions, and offer emotional support, making the experience less stressful for you. 7. Prepare for Post-Appointment CareDepending on the diagnosis, your doctor might recommend a follow-up plan for managing your ovarian cyst. This could involve monitoring the cyst over time, lifestyle changes, or medication. In some cases, surgery may be necessary, especially if the cyst is large or causing severe symptoms.Make sure you fully understand the next steps before leaving the appointment. Clarify how and when you should follow up with your doctor, what symptoms to monitor, and whether any lifestyle changes are needed to improve your reproductive health. ConclusionPreparing for your doctor’s appointment regarding ovarian cysts can help you feel more in control of your health. By organizing your medical history, knowing your symptoms, and preparing the right questions, you ensure that you get the most out of your consultation. At Marinas Clinic in Chennai, you are in expert hands with professionals like Dr. Preethi Mrinalini, known for her expertise as one of the best female surgeons in Chennai. Remember, the more prepared you are, the more confident you’ll feel in managing your health and any next steps in your treatment plan. Recent Posts The Psychological Impact of Ovarian Cysts: Coping Strategies and Support Resources 23 Sep 2024 How to Prepare for Your Doctor’s Appointment Regarding Ovarian Cysts 23 Sep 2024 How to Prevent Diabetic Foot Complications: Practical Tips from Experts 16 Sep 2024 Yoga and Haemorrhoids: Poses That Can Help Relieve Symptoms 16 Sep 2024 Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai 10 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
How to Prevent Diabetic Foot Complications: Practical Tips from Experts

Peripheral Vascular Disease: Understanding the Symptoms and Risk Factors Diabetes, a condition that affects millions globally, poses various health risks if not managed properly. One of the most significant and often overlooked complications of diabetes is diabetic foot problems, which can lead to serious consequences if not addressed early. According to Dr. Preethi Mrinalini, a leading surgeon at Marinas Clinic and widely recognized as the best female surgeon in Chennai, preventing diabetic foot complications requires a proactive approach with practical measures. By understanding the importance of foot care and incorporating expert advice into daily routines, individuals with diabetes can significantly reduce the risk of severe foot complications. Understanding the Risks of Diabetic Foot ComplicationsDiabetic foot complications arise primarily due to two factors: neuropathy (nerve damage) and poor circulation. Over time, high blood sugar levels can damage the nerves, causing a loss of sensation in the feet. This means that minor injuries, cuts, or blisters may go unnoticed and untreated, leading to infections. Poor circulation also slows down the healing process, making it harder for the body to recover from wounds, and in severe cases, can lead to ulcers or even amputations. 1. Daily Foot InspectionsThe first and most crucial step in preventing diabetic foot complications is to check your feet daily. Since diabetic neuropathy can result in a loss of feeling, it’s vital to visually inspect your feet for any signs of injury. Look for cuts, blisters, redness, or swelling. If you cannot see the bottoms of your feet easily, use a mirror or ask someone to help you.Experts recommend paying close attention to any changes in skin color or texture. Even small cracks in the skin or dry patches can lead to more severe issues if left untreated. If you notice anything unusual, it’s essential to consult a healthcare professional immediately. 2. Keep Feet Clean and MoisturizedMaintaining foot hygiene is critical in preventing infections. Wash your feet daily with warm water and mild soap, ensuring to dry them thoroughly, especially between the toes. However, avoid soaking your feet for long periods, as this can cause the skin to dry out.After washing, apply a moisturizing lotion to your feet to prevent cracking, but be sure to avoid the spaces between your toes, as excess moisture can lead to fungal infections. Regular moisturizing keeps the skin soft and helps protect it from becoming dry and prone to injury. 3. Wear Proper FootwearWearing appropriate footwear is one of the most effective ways to prevent diabetic foot complications. Shoes that are too tight, loose, or don’t offer enough support can cause blisters, calluses, or other injuries. Invest in shoes designed specifically for diabetics, which provide cushioning and support without irritating the skin.Additionally, avoid walking barefoot, even indoors. Small objects on the ground, such as pebbles or glass, can cause injuries that might go unnoticed. Diabetic socks, which are designed to reduce pressure and promote circulation, are another valuable investment for added protection. 4. Manage Blood Sugar LevelsOne of the root causes of diabetic foot complications is poorly controlled blood sugar. High blood sugar can damage blood vessels and nerves, increasing the risk of foot problems. Keeping blood sugar levels within the target range not only prevents nerve damage but also improves overall circulation, promoting faster healing.Work closely with your healthcare provider to monitor and manage your blood sugar through a combination of medication, diet, and exercise. Regular check-ups ensure that any signs of neuropathy or circulation issues are detected early, reducing the risk of complications. 5. Stay Active and Maintain Healthy CirculationRegular physical activity improves circulation, which is essential for preventing diabetic foot complications. Poor circulation can delay healing and increase the risk of infections. Walking, swimming, and cycling are all excellent forms of low-impact exercise that promote good blood flow to the feet.However, it’s important to avoid activities that put excessive pressure on your feet or increase the risk of injury. Always wear proper footwear during exercise, and consult your doctor before starting a new fitness regimen. 6. Quit SmokingSmoking narrows blood vessels, restricting blood flow to the feet and increasing the risk of complications for people with diabetes. If you smoke, quitting is one of the most significant steps you can take to protect your feet and overall health. Improved circulation allows for faster healing and reduces the likelihood of developing ulcers or infections. 7. Regular Check-ups with Your Healthcare ProviderIn addition to daily self-care, regular visits to a healthcare provider are essential in preventing diabetic foot complications. Podiatrists or surgeons can examine your feet for early signs of issues and provide expert advice on foot care. Early detection of problems like infections or ulcers can prevent them from progressing to more severe conditions.If you have any concerns about your foot health, scheduling regular check-ups with specialists like Dr. Preethi Mrinalini at Marinas Clinic is essential. Professional care ensures that potential complications are caught and treated early, minimizing risks. ConclusionPreventing diabetic foot complications requires consistent care and vigilance. By following these expert tips — inspecting your feet daily, wearing proper footwear, managing blood sugar, staying active, and consulting with healthcare providers — you can significantly reduce the risk of serious complications. For those living in Chennai, Dr. Preethi Mrinalini, known as the best female surgeon in Chennai, offers specialized care in managing diabetic foot health. Prioritizing your foot care today can help you maintain an active, healthy lifestyle and avoid complications in the future. Recent Posts How to Prevent Diabetic Foot Complications: Practical Tips from Experts 16 Sep 2024 Yoga and Haemorrhoids: Poses That Can Help Relieve Symptoms 16 Sep 2024 Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai 10 Sep 2024 Frequently Asked Questions About Laparoscopic Surgeons: What Patients Should Know 09 Sep 2024 Top 5 Non-Surgical Lipoma Treatment Options You Should Know 02 Sep 2024 Have Any Question? Contact us +91 98840 00171 [email protected]
Yoga and Haemorrhoids: Poses That Can Help Relieve Symptoms

Peripheral Vascular Disease: Understanding the Symptoms and Risk Factors Haemorrhoids, commonly known as piles, are swollen veins in the rectal area that cause discomfort, itching, and pain. They affect millions of people worldwide, and while medical treatments are available, holistic approaches like yoga can also play a significant role in alleviating symptoms. Practicing certain yoga poses can improve circulation, reduce inflammation, and ease constipation, which is often one of the leading causes of haemorrhoids.According to Dr. Preethi Mrinalini, a renowned surgeon at Marinas Clinic and regarded as the best female surgeon in Chennai, incorporating yoga into a lifestyle routine can be beneficial for haemorrhoid management. While medical treatment should always be a priority, yoga offers a gentle, non-invasive method to relieve symptoms and promote overall well-being. How Yoga Helps with HaemorrhoidsYoga is known for its ability to increase blood flow, reduce tension, and support better digestion. When practiced mindfully, it can help ease some of the underlying causes of haemorrhoids, such as constipation and prolonged sitting. The deep breathing techniques and movements associated with yoga encourage relaxation in the muscles, which helps prevent the strain that can worsen haemorrhoids.Certain yoga poses are particularly useful for enhancing bowel movement, improving circulation, and reducing pressure in the rectal area. Below are a few yoga poses that can be particularly effective for relieving haemorrhoid symptoms. 1. Malasana (Garland Pose)Malasana is a deep squat that stretches the lower back, hips, and groin while also stimulating the digestive organs. This pose helps with constipation by increasing bowel movement, which in turn reduces the pressure on haemorrhoids.How to do it: Stand with your feet slightly wider than hip-width apart. Slowly squat down, bringing your torso between your thighs. Keep your hands in a prayer position and your elbows pressing into your knees to open your hips. Hold the pose for 30 seconds to a minute, focusing on deep breathing. 2. Pawanmuktasana (Wind-Relieving Pose)Pawanmuktasana is designed to release trapped gas and promote digestion, making it ideal for people suffering from haemorrhoids due to constipation. This pose massages the abdominal organs, promoting better bowel movement and reducing inflammation.How to do it: Lie on your back with your legs extended. Slowly bring one knee toward your chest, hugging it tightly with both hands. Hold for a few breaths, then switch to the other leg. You can also bring both knees to your chest for a deeper stretch. Hold the pose for up to a minute on each side. 3. Balasana (Child’s Pose)Child’s Pose is a gentle resting position that helps reduce stress and calm the nervous system. By promoting relaxation and reducing stress, it indirectly eases haemorrhoid symptoms, which are often exacerbated by tension and anxiety.How to do it: Kneel on the floor with your big toes touching and your knees spread apart. Lower your torso between your thighs, extending your arms forward or resting them by your sides. Rest your forehead on the floor and breathe deeply for 1-2 minutes. 4. Viparita Karani (Legs-Up-the-Wall Pose)This restorative pose helps improve circulation and reduces the pressure on the rectal veins. By elevating your legs, it allows blood to flow away from the lower body, alleviating discomfort and swelling in the haemorrhoid-affected area.How to do it: Sit with your right side against the wall, then gently swing your legs up as you lower your back to the floor. Keep your legs vertical against the wall and rest your arms by your sides. Relax in this position for 5-10 minutes, focusing on slow, deep breaths. 5. Paschimottanasana (Seated Forward Bend)This pose stretches the entire back of the body, promoting relaxation and stimulating digestion. It helps relieve constipation, a common cause of haemorrhoids, by massaging the abdominal organs and encouraging bowel movements.How to do it: Sit with your legs extended in front of you. Inhale and lengthen your spine, then exhale and fold forward, reaching for your feet. Keep your spine as straight as possible, and hold the pose for 1-2 minutes, focusing on deep breathing. 6. Baddha Konasana (Bound Angle Pose)This pose opens the hips and stimulates the abdominal organs, promoting better digestion and reducing the discomfort associated with haemorrhoids. It also improves circulation in the pelvic area, which can help relieve symptoms.How to do it: Sit with your legs extended in front of you. Bend your knees and bring the soles of your feet together, letting your knees drop to the sides. Hold your feet with your hands, and sit up tall, focusing on your breath for 1-2 minutes. Precautions and TipsWhile yoga can provide relief, it is important to practice the poses mindfully. Avoid positions that strain the rectal area or require excessive effort. Start slowly and focus on gentle poses that promote relaxation and improved digestion. Remember to listen to your body and avoid pushing yourself beyond your comfort level.Incorporating yoga as part of a comprehensive treatment plan for haemorrhoids can be highly effective, but it’s always important to consult a healthcare professional before starting any new exercise routine, especially if you are already experiencing discomfort. ConclusionYoga can be a valuable addition to traditional haemorrhoid treatments, helping to relieve symptoms and improve overall well-being. By practicing poses that reduce stress, enhance circulation, and promote digestion, individuals can experience significant relief from haemorrhoid discomfort. While these poses are beneficial, it’s crucial to combine them with proper medical care, especially for more severe cases. As Dr. Preethi Mrinalini at Marinas Clinic, one of the best female surgeons in Chennai, advises, a balanced approach that includes both medical treatment and lifestyle changes like yoga can offer the best outcomes for patients dealing with haemorrhoids. Recent Posts How to Prevent Diabetic Foot Complications: Practical Tips from Experts 16 Sep 2024 Yoga and Haemorrhoids: Poses That Can Help Relieve Symptoms 16 Sep 2024 Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai 10 Sep 2024 Frequently Asked Questions About Laparoscopic Surgeons: What Patients Should Know 09 Sep 2024 Top 5 Non-Surgical Lipoma Treatment Options You Should Know 02 Sep 2024 Have Any
Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai

Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai When it comes to selecting a surgeon for complex medical procedures, expertise, experience, and compassion are essential qualities. Dr. Preethi Mrinalini K, a consultant surgeon at Apollo Hospitals, Greams Road, and Marina’s Clinic in Nungambakkam, Chennai, has earned a reputation as one of the finest female surgeons in the city. Specializing in laparoscopic, bariatric, and gastrointestinal surgeries, Dr. Preethi brings over 12 years of experience to her practice, combining advanced medical techniques with a patient-centered approach.An Exceptional Journey in Medical PracticeDr. Preethi Mrinalini K’s remarkable journey began with her medical education at Sri Ramachandra Medical College in Chennai, where she completed her MBBS and later earned her MS in General Surgery. Her passion for surgery and continuous learning led her to further specialize in minimally invasive techniques, particularly laparoscopic and bariatric surgery. She completed her fellowship in Metabolic and Bariatric Surgery (FMBS) and later became a Fellow of the Indian Association of Gastrointestinal Endosurgeons (FIAGES), solidifying her credentials as one of the leading surgeons in Chennai.Her extensive training and hands-on experience have equipped her with the knowledge to perform complex gastrointestinal procedures with precision and skill. Whether it’s performing surgeries for weight loss, treating hernias, or addressing gastrointestinal issues, Dr. Preethi’s patients benefit from her holistic approach that ensures both surgical excellence and comprehensive patient care.A Leader in Laparoscopic and Bariatric SurgeryOne of Dr. Preethi’s key areas of expertise lies in laparoscopic surgery. Laparoscopic procedures involve small incisions, leading to quicker recovery times, less pain, and minimal scarring. This makes them a preferred option for patients who want to return to their normal routines as soon as possible. As one of the best laparoscopic surgeons in Chennai, Dr. Preethi has successfully performed numerous surgeries using this advanced technique. Whether it’s gallbladder removal, appendectomies, or more complex gastrointestinal procedures, Dr. Preethi’s skills ensure that patients experience fewer post-operative complications and faster recovery.Her specialization also extends to bariatric surgery, where she has helped many patients manage obesity and its associated conditions through minimally invasive techniques. As a certified bariatric surgeon with FMBS credentials, Dr. Preethi has proven her ability to provide long-term weight loss solutions for patients, improving their quality of life and reducing health risks.Commitment to Patient-Centered CareWhat sets Dr. Preethi apart is not only her technical skills but also her unwavering commitment to her patient’s well-being. At both Apollo Hospitals, Greams Road, and Marina’s Clinic in Nungambakkam, she dedicates her time to offering personalized care to each patient. Her daily availability—10 am to 2 pm at Apollo Hospitals and 5 pm to 8 pm at Marina’s Clinic—ensures that patients have access to her expertise at their convenience.Dr. Preethi believes in a patient-first approach. She takes the time to listen to her patients, understand their concerns, and educate them on their treatment options. Whether it’s a consultation before surgery or guidance on post-operative care, she ensures that her patients feel comfortable and confident in their treatment journey. This transparent and compassionate care has made her a trusted name among patients, particularly women who seek a surgeon with a deep understanding of their medical needs.Why Choose Dr. Preethi Mrinalini?Choosing the right surgeon is crucial for any procedure, especially when it involves sensitive gastrointestinal and metabolic conditions. Dr. Preethi’s combination of education, experience, and dedication to excellence makes her an ideal choice for anyone in need of gastrointestinal surgery. Extensive Education and Training: With specialized training in laparoscopic and bariatric surgeries, Dr. Preethi offers the most advanced surgical techniques available. Her extensive knowledge in gastroenterology ensures that every patient receives the best care possible, leading to excellent results. Professional Accomplishments: Her expertise is reflected in the numerous successful surgeries she has performed. From complex gastrointestinal cases to laparoscopic procedures, Dr. Preethi’s track record speaks to her surgical precision and patient outcomes. Holistic Patient Care: Dr. Preethi is committed to providing comprehensive care from pre-operative consultations to post-operative follow-ups. This patient-centered approach ensures that every individual feels supported and informed throughout their treatment journey. Minimally Invasive Techniques: As one of the best laparoscopic surgeons in Chennai, Dr. Preethi focuses on using minimally invasive approaches to reduce recovery times, pain, and scarring for her patients. Her laparoscopic and bariatric surgeries are known for producing excellent outcomes with fewer complications. Professional Dedication and ExperienceOver the course of her 12+ year career, Dr. Preethi has built a strong reputation for handling complex cases with confidence and skill. Her experience allows her to manage even the most challenging scenarios with precision, ensuring successful surgical outcomes. Patients who have undergone procedures with Dr. Preethi often speak highly of her professionalism, skill, and compassionate bedside manner.ConclusionDr. Preethi Mrinalini K’s extensive medical knowledge, surgical skills, and commitment to patient care have firmly established her as one of the best female surgeons in Chennai. Whether you are considering bariatric surgery, gastrointestinal treatment, or laparoscopic procedures, Dr. Preethi’s experience and patient-centered approach make her the ideal choice. At Marina’s Clinic and Apollo Hospitals, patients can trust that they are receiving world-class care from a leading expert in the field. If you’re looking for the best female surgeon in Chennai, Dr. Preethi Mrinalini is a name you can trust. Recent Posts Dr. Preethi Mrinalini K: The Best Female Surgeon in Chennai 10 Sep 2024 Frequently Asked Questions About Laparoscopic Surgeons: What Patients Should Know 09 Sep 2024 Top 5 Non-Surgical Lipoma Treatment Options You Should Know 02 Sep 2024 An Interview with a Gastroenterologist on Anal Fissure Treatments 02 Sep 2024 Lipoma or Something Else? How to Identify and Differentiate Skin Lumps 26 Aug 2024 Have Any Question? Contact us +91 98840 00171 [email protected]

